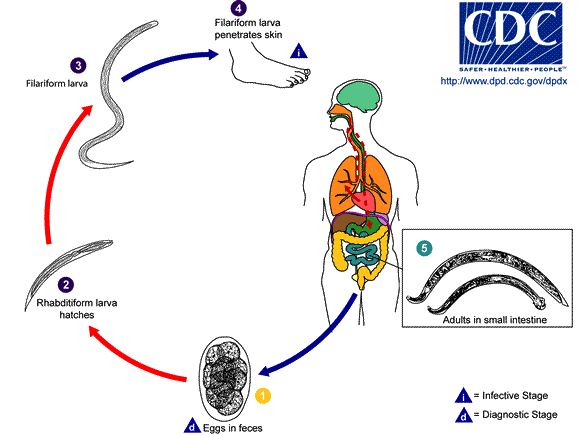
For people with serious autoimmune diseases the outlook is generally dim. They are told by their medical providers that there is nothing to be done about the disease except “manage” devastating symptoms with powerful immune suppressing drugs that foster serious side effects. As I mentioned in my previous post about our Old Friends and the Hygiene Hypothesis, there is some very exciting human trials going on right now investigating the efficacy of parasitic infection with helmiths as a potential therapy for autoimmune conditions.
Probiotics have gotten attention
Most conventional medical providers never consider that diseases start in the gut, as Hippocrates stated so many years ago, because they are trained to write prescriptions.
However, in the last few years there have been studies with many strains of our friendly gut bacteria that show promise as therapeutic modalities for certain conditions. Probiotics are always recommended by nutrition professionals as a mainstay therapy but probiotics are not the whole story. Our intestinal tract is home to many different species of bacteria, as well as viruses, yeasts and even worms.
More recently, soil based organisms (also bacterial species with remnants of soil particles like humic and fulvic acid) are also subjects of interest in recalcitrant autoimmune conditions.
Parasites are usually reviled
Upon stool sampling, pathogenic varieties of microorganisms may be identified and the reaction would be to try to eradicate them with herbal combinations or even medications. But we are finding out that not all parasites are bad. In fact, when they are in low levels, there are some that may be beneficial, especially to those with autoimmunity.
Of course, any large infection with a lot of parasites would have to be resolved with medications, but many light infections are not even treated by medical doctors. Perhaps those people are the lucky ones — perhaps a light infection is just what is needed to prevent autoimmunity.
The hygiene hypothesis
Because of modern sanitation and technology we have eliminating typhoid and cholera and have saved millions of lives, since sewers and clean drinking water were introduced in North American and Western Europe. But in doing so, we have contributed to the rise of the modern diseases involving immune dysregulation, like multiple sclerosis, Crohn’s, ulcerative colitis, Graves disease, Hashimoto’s thyroiditis, Type I diabetes, asthma, allergy, celiac disease, and Sjogren’s syndrome to name just a few.
In our super sterilized world we have removed many sources of microorganisms, both beneficial and disease causing. We are supposed to have many different types of organisms living with us — that have been there for over 10,000 years.
Hygiene Hypothesis is the basis for this research
Based on this hygiene hypothesis, researchers at the University of Iowa wanted to find a safe parasite—one that wasn’t known to cause infection or illness in humans—for therapeutic purposes. This particular helminthic treatment, is pig whipworm or TSO from the Latin name for whipworm eggs: Trichuris Suis Ova. TSO, the microscopic eggs of the porcine whipworm, is a novel, orally administered, natural immunomodulator that regulates T-Cells and pro-inflammatory cytokines.
TSO was chosen as the biological agent of choice because it is not a human pathogen and is spontaneously eliminated from the body within several weeks after dosing. Additionally, T suis ova remain isolated to the gastrointestinal tract. The ova may be obtained under pathogen-free conditions and may be stored for 2 years. Furthermore, if any adverse affects occur, termination of the therapy is fast and simple with oral antihelminthic agents.
Effects of the parasite Trichuris suis (pig whipworm) is studied in ulcerative colitis
In 2003 Summers, R, et al studied 7 people, 4 with Crohn’s and 3 with colitis. They were each given a single dose of Trich suis ova and were followed for 12 weeks. According to the IBD Quality of Life Index, six of seven patients (86%) achieved remission. The researchers concluded that the therapy was safe to use with patients with Crohn’s disease and ulcerative colitis and that the findings suggest that it is possible to down regulate intestinal inflammation in humans with helminths.
In 2005 one of the researcher at the forefront of helminth research, Dr. Joel Weinstock, did a study entitled, Trichuris suis therapy for active ulcerative colitis: a randomized controlled trial. This study involved 54 patients with active ulcerative colitis. They were randomly given either placebo or Trichuris suis ova.
After 12 weeks they were evaluated using the Disease Activity Index to > or = 4. They found that 43.3% of the treated group had significant improvement compared to 16.7% of the placebo group. Improvement was also found with the Simple Index that was significant by week 6. Treatment induced no side effects.
Their conclusions were that T suis ova therapy seemed safe and effective in patients with active colitis.
Trichuris Suis Therapy in Crohn’s Disease
In 2005 Summers, RW, et al published a study called Trichuris Suis Therapy in Crohn’s Disease in the journal Gut. Twenty nine patients with active Crohn’s disease, defined by a Crohn’s disease activity index (CDAI) were enrolled in this open label study.
All patients ingested 2500 live T suis ova every three weeks for 24 weeks, and disease activity was monitored by CDAI. Remission was defined as a decrease in CDAI to less than 150 while a response was defined as a decrease in CDAI of greater than 100.
At week 24, 79.3% responded and 21/29 (72.4%) achieved remission (CDAI <150). Mean CDAI of responders decreased 177.1 points below baseline. An analysis conducted at week 12 yielded similar results. There were no adverse events.
The researcher concluded,
This new therapy may offer a unique, safe, and efficacious alternative for Crohn’s disease management. These findings also support the premise that natural exposure to helminths such as T suis affords protection from immunological diseases like Crohn’s disease.
More promising results with TSO
More recently, Coronado Biosciences, Inc. a biopharmaceutical company focused on the development of novel immunotherapy agents for the treatment of autoimmune diseases and cancer, just announced in April 2012, that they will continue with phase 2 clinical trials in Europe evaluating Trichuris suis ova in Crohn’s disease. The phase 1 trials showed positive results with TSO in patients with Crohn’s disease, where TSO was shown to be safe and well tolerated. The Phase 1 trial was a multi-center, sequential dose, dose-escalation, double-blind, placebo-controlled study of 36 patients with Crohn’s disease.
Called The Falk Trial, this new phase is a double-blind, randomised, placebo-controlled, multi-center phase II study to evaluate the efficacy and safety of three different dosages of oral Trichuris suis ova (TSO) suspension in active Crohn’s disease. It is being conducted in Europe and was initially expected to enroll approximately 212 patients and to evaluate three different dosages of TSO versus placebo.
This is very promising and exciting for those interested in this therapy.
Effects of the parasite hookworm is studied in Celiac disease
In the Princess Alexandra Hospital in Brisbane Australia, a Phase 2 clinical trial in humans was conducted for Celiac disease, entitled, Suppression of Inflammatory Immune Responses in Celiac Disease by Experimental Hookworm Infection, lead by McSorley, HJ, et al. Here is a synopsis of the study:
This was a two stage clinical trial. In trial one, there were 20 participants in total with Celiac — all on a gluten-free diet. Ten were randomly infected with the larva of the hookworm (Necator americanus) administered via the skin. The controls were given topically administered chilli pepper (to mimic the typical skin reaction when hookworm is administered). At 20 weeks post-infection (with a top-up at 5 weeks), a gluten-challenge was given.
In Trial Two, seven of the control participants were infected with hookworm, with the same top-up infection and gluten challenge.
Results showed that levels of duodenal interferon-gamma (IF-y) and the cytokine IL-17A (inflammatory cytokines) were significantly decreased in the hookworm infected group from Trial 1 post gluten challenge.
This and other cytokine indicators led the authors to hypothesize that helminth therapy might skew the immune response in Celiac towards a Th2 phenotype; in effect, a more anti-inflammatory response (see this article for a better description of Th1 and Th2).
Multiple Sclerosis
In the Journal of Immunology 2009 Nov 1;183(9):5999-6012, a study was published that found that helminth molecules exert potent regulatory effects on both dendritic cells and B cells through TLR2 regulation conducted via different signaling pathways. (Dentritic cells and B cells are cells involved in the immune response). The researchers conclude that “…this knowledge could prove critical in developing novel therapeutic approaches for the treatment of autoimmune diseases such as MS.”
In a study published in the Annals of Neurology in 2007 with a 4.6 year follow-up, researchers found that parasite infected MS patients showed a significantly lower number of exacerbations, minimal variations in disability scores and minimal changes to their MRIs when compared with uninfected MS patients.
What this means is that the helminth infection protected the MS patients from getting worse.
Another study in 2008 published in the Annals of Neurology by the same researchers as above, (Jorge Correale, et al), set out to assess the importance of B-cell control during parasite infections in multiple sclerosis (MS) patients.
They found that helminth infections in MS patients created a B-cell population producing high levels of IL-10, dampening harmful immune responses. Moreover, B cells isolated from helminth-infected MS patients also produced greater amounts of brain-derived neurotrophic factor and nerve growth factor compared with those of normal subjects, raising the possibility that these cells may exert a neuroprotective effect on the central nervous system.
Asthma
In a dose-ranging study for asthma in 2006, Mortimer, et al found that a dose as little as 10 Necator Americanus (hookworm) produced mild changes in immune cells, but no changes in lung function. They did note that as the dose went up, side effects did emerge. Hookworm is known to cause some gastrointestinal discomfort, and skin itching and rash at the entry site. These are transient. The researcher concluded that N. Americanus is potentially suitable for use in preliminary clinical therapeutic trials.
Other mechanisms of action being suggested
In the journal, Trends in Parasitology (a good bedtime read) in 2012, Martin J. Wolff (NYU) , Mara J. Broadhurst and P’ng Loke (NYU) published a review entitled, Helminthic therapy: improving mucosal barrier function. Here they reviewed much of the current research with helminths. Most of the researchers suggest that the helminths dampen the overactive parts of the immune system by inducing T regulatory cells. Wolff, et al are suggesting that there is also another mechanism by which the worms reduce inflammation. That is, that the worms may enhance mucosal barrier function and this plays an important role in improving conditions of inflammatory bowel diseases.
Some of the cytokines activated by the helminths increase goblet cell hyperplasia and mucus production, and increase turnover of intestinal epithelial cells. The researchers propose that these alterations in the mucosal barrier in the gut may play a protective role against pathology and may potentially be as important as immune regulation in modulating the inflammatory response.
A common thread of results
Are you beginning to see the common thread of results here? There have been significant improvements in patients documented in every single study. Some have shown major improvements in people with autoimmune disorders — and this is a big one — there are no significant side effects with this treatment.
What could be more natural than repopulating the gut with organisms that we co-evolved with — organisms that should be there — but for the scourge of modern life. Maybe we need to run and play in the mud more often!
Stay tuned for more about our old friends and what some people with other autoimmune conditions as well as autism (which some consider to be an autoimmune condition) are doing with this information about helminths.
Related articles:
- The AutoImmune Crisis: What To Do About It
- Old Friends: The Hygiene Hypothesis
- 8 Reasons to Add Probiotics to Your Diet
- Probiotics: The New Therapeutic Frontier
Further Information: